News
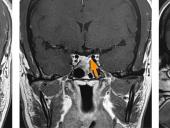
Recently, a patient with acromegaly — a condition that often results from a hormone-secreting tumor in the pituitary gland — arrived at UCSF's California Center for Pituitary Disorders. She had undergone what appeared to be a successful surgical resection of her tumor, but the condition persisted and she was hoping to avoid the radiation therapy her physicians recommended.
On May 1, 2017 the California Center for Pituitary Disorders at UCSF celebrates its 10-year anniversary! In that time neurosurgeons at UCSF have performed 2,110 microscopic and endoscopic transsphenoidal surgical procedures to remove pituitary tumors. The CCPD now averages 240 operations and over 2,000 outpatient visits annually, making it one of the most active and specialized pituitary treatment centers in the nation.